My recent experience with triple bypass open heart surgery taught me a lot about how to stay healthy.
 Jeff Nightbyrd will be Thorne Dreyer’s guest on Rag Radio, Friday, Feb. 27, 2015, 2-3 p.m. (CST), on KOOP 91.7-FM in Austin and streamed live. Jeff will discuss issues related to this article.
Jeff Nightbyrd will be Thorne Dreyer’s guest on Rag Radio, Friday, Feb. 27, 2015, 2-3 p.m. (CST), on KOOP 91.7-FM in Austin and streamed live. Jeff will discuss issues related to this article.
UPDATE: Listen to or download the podcast of our Rag Radio interview with Jeff Nightbyrd here:
Last year I had open heart, triple bypass surgery. Kind of takes the wind out of your sails. But I am recovering remarkably well so the prognosis is another 20 years of normal energetic life instead of sudden death. Because this surgery is becoming common — there will be more than 150,000 such procedures in the U.S. this year — some of you or your loved ones will be facing this scary reality. So I thought I would share some helpful lessons I learned the hard way.
Your heart
Your heart will beat about 42 million times this year. That’s a stunning amount of work. An average person can fill up 12 swimming pools with blood in a year. OK, I just made up that statistic but you get the idea. In the time you took to read this far your heart has pumped about a gallon of blood.
Your heart will beat close to three billion
times in your life.
Your heart will beat close to three billion — that’s billion with a “B” — times in your life. (I didn’t make that up.) Ball up your fist. Look at it. That’s the size of your heart. That small little muscle performs a hideous amount of work keeping you alive. So you need to care for it.
The good news is in about seven years your body replaces all its cells. So if you make positive lifestyle changes it will show up in every organ of your body. You can basically have a new heart, cell by cell, in seven years, so bad habits can be redeemed.
Diagnostic failure
Americans are great surgeons or, as my cardiac rehab nurse likes to call them, “great plumbers.” These great surgeons are poor at seeing the whole person. My Chinese doctor looks at my tongue, my eyes, even my fingernails, takes eight different pulses, watches posture, and without being obvious smells my body. For diagnosis, American cardiologists rely on computer printouts of various tests.
In my particular case, I ate fairly well, was lean and in reasonable shape. My yearly checkups showed normal blood cholesterol levels. My blood oxygen level at my fingertips ran 98%. I complained of feeling more fatigue and was always reassured, “You’re getting older.”
Looking back, there were clear danger signs.
But looking back, there were clear danger signs. My father died of a heart attack at 48. I had high blood pressure and a too-quick pulse. My persistent hacking cough over four months this spring was chalked up to allergies (even though the heart and lungs are intimately related). Even after having one heart attack followed by two minis, one cardiologist judged, “Fifty-fifty you didn’t have a heart attack.” He thought maybe there was a false positive on the heart attack enzyme test and recurring bouts of acid reflux.
But, when I went in for an angioplasty (your arteries are injected with dye) and stents, the truth came out. One artery to my heart was 96% occluded. Even though groggy, I saw on the monitor an hourglass shape with a thin string where blood was supposed to flow and remember the doctors saying: “Let’s bring him up and talk about our options.”
Severely stoned on anesthetics, I still knew this comment wasn’t what they call “a good indicator.”
An hour later in the option discussion I said, “I always favor the nutritional approach.” One cardiologist replied, “There’s nothing wrong with the nutritional approach. However you’ll be dead before it has time to take effect.”
So… triple bypass time.
I was at the stage where, without warning,
you keel over dead.
I was at the stage where, without warning, you keel over dead. I had the classic “widow-maker” artery. The diagnostics had failed. The blood cholesterol tests were normal because my body was excellent at taking cholesterol and attaching it to my artery walls and not letting it float around my bloodstream. Nothing alarming showed up on standard blood tests.
TIP: The standard cholesterol tests are 20 years dated and inadequate. You want to get a VAP test which gives you 19 important cholesterol and lipid readings and is much more informative about your true condition. It’s the new standard and costs about $100. If in doubt about your heart, be sure to get a VAP test.
Your danger
Some of you are walking around with the potential of crippling heart attacks and the standard tests are not giving you warning signals. I look at friends with an unhealthy pallor and bloated skin (edema from too much salt) and think, “They might die.” The lesson is: You’ve got to know your body better than the doctor who gives you yearly checkups because the American corporate medical approach is weak in diagnostics.
There will be 150,000 bypass operations this year and many more insertions of stints into coronary arteries. Believe me you want to avoid life threatening open-heart surgery and even stints. As you’ve heard countless times, most heart problems are preventable through an intelligent diet, exercise, and most critically — not smoking.
Information is power
Information about what is going to happen during surgery eases the mind. Ask all your friends about their family’s experience. Read, watch YouTube, and get personal stories so you know what to expect. The only two persons I met who had a family member die reported it was due to staph infections picked up in the hospital. My sister, a nurse, said, “I’ve assisted in about 60 bypasses. We didn’t lose anybody.” That was reassuring.
I asked the surgeon about the fatality rate and he replied, “About 5%.” (A high number.) I think he wanted me to take the pre-op preparation seriously
Bottom line, if you are basically healthy you should make it through OK.
They cut you open like a supermarket-packaged, split chicken breast.
But remember, the operation includes sawing your sternum in half. They cut you open like a supermarket-packaged, split chicken breast. At home a week later, each cough is like being stabbed in the chest with a knife — maybe a pain level of 9 on a scale of 10 — and at 10 you pass out. The good news is that within a few days a cough or laugh drops down to a 7 — which is like like being stabbed with a sharp knife, not the rusty serrated blade that yields a 9.
Post-surgery
During the first week out of the hospital you will need friends with you 24 hours a day. I feel like my friends were lifesavers. For instance, at night you wake up and need to make it to the bathroom. But sitting or standing quickly makes you dizzy.
Fall on your head, and the mega dose of blood thinner coursing through your arteries, will make your brain hemorrhage like an unscrewed fire hydrant. The EMS would need to get you to surgery quickly to relieve the blood choking your brain.
Or if you didn’t crack your head on the floor in a fall, your sternum could pop apart as if ready for another open-chest surgery. The sternum popping apart is likely not life threatening, but you would pass out from the overwhelming pain. As I’ve said, during the first week at home each cough or even laugh was tortuously painful — even with painkillers. Having a friend press a pillow to your chest, almost full strength, is the only thing that brings relief.
Surgery and the American way
Doctors from various healing traditions have told me, “Americans are great with surgery.” And indeed they are. Think about this: The heart surgeon takes a vein that’s removed from your leg about the width of a string of yarn. Then it is sewed with micro stitches into two incisions in your heart, by-passing the clogged artery. The graft has to be perfect. When the heart is reanimated and beating again there can be no blood leakage around the repair. But the vein can’t be sewed in too tight. Too-tight stitching will make the raw ends heal together and no blood will flow. The surgery has to be perfect.
The aftercare by the heart team doctors consists mostly of reading test results and
prescribing pills.
So the surgery is great. But the aftercare by the heart team doctors consists mostly of reading test results and prescribing pills. They follow standard protocol. I take something like eight different pills, which is normal. Studying each one on Google, it’s clear they all have side effects. In the case of the most effective arrhythmia medication, it’s potentially lethal.
Getting off the pills is much more difficult than getting them prescribed. Because each person’s body is unique, a patient in recovery needs to read extensively and figure out what medications may not be working effectively, or are causing too many side effects. Our medical system’s post-op care simply doesn’t have the continuity and holistic view to do a good personal job. Because I’ll live, I’m not a statistical problem for the system that requires unusual attention. This isn’t ideal for you, if post-op you are trying to maximize your quality of life.
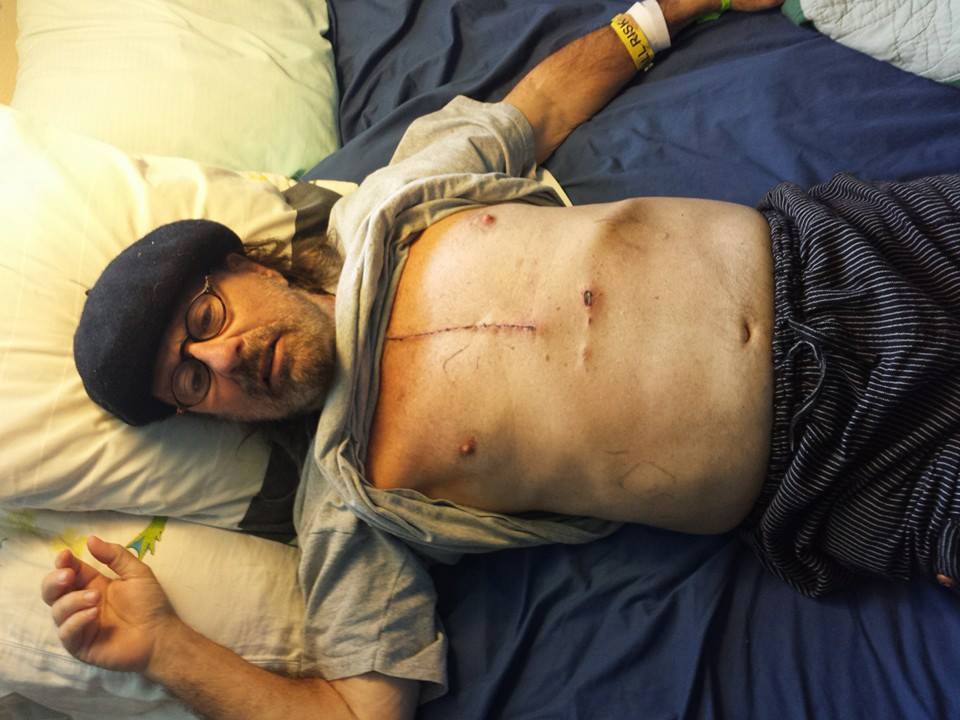
For instance, various drainage tubes were extracted from my chest (see video). One hole, looking like a bullet wound, wasn’t healing well. On each of a half dozen visits to the cardiologists, they would remark: “That doesn’t seem to be healing well.” End of story. They were cardiologists, surgical specialists, and not one stuck his nose or a Q tip anywhere near the hole.
When I visited the physical rehab nurse five weeks after surgery, she looked at my hole and said, “That looks bad. Let’s fix it up.” She got out saline, gauze, and a probe and started cleaning out dead tissue.
“That would take a while to heal if you hadn’t cleaned it,” I said.
She replied, “It would never have healed with all that dead tissue in there. You would have had a hole and at some point you would develop a serious infection.”
Underneath, the hole stretched an inch and a half in every direction. The physical rehab nurse saw me as a whole body and had a practical approach to fixing things. The surgery team was too focused on cardiac surgery to treat an open wound. And as surgical specialists they also weren’t good at answering basic questions like what was the recommended diet for me?
“Oh, just use your common sense!” was the answer.
The featured entrees were barbeque pork sandwiches and ribeye steaks.
At Seton Hospital in Austin I happened to visit the staff cafeteria. The featured entrees were barbeque pork sandwiches and ribeye steaks. No Joke!
A man in a chef’s outfit and a pushcart passed among the diners baking lunch plate-sized chocolate chip cookies. In recovery, I was served that pseudo fruit juice — two percent juice, colored water, and artificial sweetener. My friends brought me food from the local health food store. I would tell the doctors, “This hospital’s idea of food is stuck in the 1950s.” They would laugh and say “Everyone thinks it’s terrible.”
End of story.
Wait! Wait! I would think, “Nutrition is part of healing.”
More than half face depression
Depression affects more than 50% of post-op patients. This is our bodies’ reaction to the drugs we are given, during and after surgery, that help us survive. Also it is the result of the intense shock of surgery. Depression should be recognized and treated immediately. Anti-depressive medication may be needed while your body tries to rebalance.
Post-op patients suffering from depression experience more physical complications.
The statistical proof is that post-op patients suffering from depression experience more physical complications. The body and mind are truly ONE. If your physical system suffers, your mind suffers. And conversely, if your mind suffers, your body suffers.
This is not Dr. Feelgood pop medicine. We humans are powerful: our thoughts create chemicals. How you construct your reality doesn’t just store neo-electrical impulses in your brain. Your thoughts constantly can and do produce chemicals, including enzymes and hormones, that regulate how you function and feel. For example, worry enough and you will soon develop indigestion. Think anxious thoughts and your heart will beat faster.
With depression, a focus on a body part can amplify pain many times. And similarly, if you are happy and excited, looking forward to something terrific, you will forget about real pains.
Cognitive decline
This is really important. Surgeons measure success by your survival. They want you healing well enough to go home without physical complications. They have a limited vision of your quality of life. But quality of life will be of the utmost importance to you and your friends. “Not dying” isn’t your goal. It’s “flourishing” at a higher level of life.
Very few heart specialists reveal to their patients that they can expect post-surgery cognitive decline. Maybe 20 IQ points down for six months? Depression — yes, for the majority of patients. But not mental decline.
One problem is the side effects from some post-surgery medications which can make you feel like a zombie. The side effects of some heart medications, particularly beta blockers, leave you barely able to think and with zero motivation to rise from bed. But the cardiologists are pleased because your ticker is ticking.
The good news is you do not have to be a zombie with a beating heart. Nor do you need six months or more post-surgery to return to good mental function. First, you need to explore the peculiarities of your body and then push the cardiologists to adjust your medications. Remember, with exercise and time you will have much more oxygen flowing to your brain (which utilizes almost a third of your blood flow).
You should or could be smarter than ever.
Lazarus rises
As I have mentioned, open heart surgery is a near-death experience. Your heart is stopped with a cold saline solution as the blood is transferred to a machine. Your lungs are also stopped. Think how desperately you want to breathe when you swim under water too long. The meta impulses, way beyond your conscience mind, scream BREATHE! BREATHE!
For an hour and a half you are as near to dead as we can get without having a funeral.
The meta program for your heart is even more intense. During surgery, if your heart warms slightly, pacemaker cells start firing spasmodically, trying to make the body live. The chemicals that are added to your cocktail of anesthetics must be tremendously powerful to shut down the the will of breath and heart beat. For an hour and a half you are dead. (Or as near to dead as we can get without having a funeral.)
Then the anesthesiologist flushes the heart-stopping chemicals from your anesthetic and your sewn-up heart is restarted. I’ve learned from some experts that anesthesia is good, but not perfect. After surgery, many of us suffer not only from depression but also from reduced mental function. Unaided, your body can take six months or more to return to norm.
This is not the realm of the cardiology specialists so much as the holistic doctors, the advanced nutritionists, and others who treat the body as a unified system (which includes the mind). From the shock of successful open-heart surgery your body literally has to relearn how to BE. The cells of mental and physical pathways that close down have to get the signal to resume their normal function.
A minor example:
At rehab, seven weeks after surgery, I was doing a simple rehab exercise to strengthen the chest muscles that connect to the sternum and which wither from lack of use. Suddenly I felt a sharp pain in my upper chest below my right clavicle . Because the heart is on the left side it didn’t seem like a surgery stitch exploded. But ever the alarmist, I felt some artery must be bursting. The pain felt like when you’ve been studying too long and your leg goes so completely asleep sitting in one position that it cuts off your circulation. Try to stand and you fall. Then a sharp pain roars through your limb as the blood starts to flow.
I was scared to tell the rehab nurse, but when I finally confessed this disaster she laughed brightly. “That’s good,” she said. “The exercises made your nerve wake up.”
After seven weeks!
Solutions
So one key is exercise. The normal heart muscle tops out at about 70% efficiency. Meaning with each beat the heart evacuates 70% of the blood in its chamber. I was at 36% efficiency prior to surgery. One artery was 96% occluded. Within a couple weeks after surgery an echo cardiogram showed my heart had improved to 46% efficiency. By doing regular physical rehab like brisk treadmill walking, you should be back in the 60% range in a few months. Your heart can heal.
There are certain vitamins, enzymes, and supplements that can speed the healing process. My goal is to be smarter and healthier than last year.
Among the supplements to consider are:
- Mitochondrial energy
- D-Ribose = muscle energy
- Ubiquinol CoQ 10
- Magnesium aspartate
- Curcumin
- Neo 40 Pro (This was just developed at the University of Texas Medical Center in Houston.)
Another good internet link is from the government: www.n/m.nih.gov/portals/healthcare.html
Also, Google everything you are taking and inform yourself about the effects, dosage, and alternatives.
My 21st generation Chinese doctor suggests blueberries and blackberries. (I buy organic because non-organic berries have among the highest pesticide residue of any fruit or vegetable sold.) The elderly acupuncturist also recommends fresh ginger tea, brewed first thing every morning, to strengthen the heart. Some credible studies indicate your tea or lemon water should be consumed a half hour before eating breakfast.
Because our bodies and metabolism differ there are few universal panaceas.
Because our bodies and metabolism differ there are few universal panaceas outside of exercise, fiber, reducing sodium — and, of course, not smoking. You need to study and learn what works for your mind and body.
Two more nutritional tips: Fiber and sodium salt
Dietary fiber might be the simplest approach to heart health.
There are many excellent research reports confirming the power of dietary fiber — particularly from grains. A recent Harvard study of 40,000 patients found high fiber intake reduced mortality among heart patients by 40%. Another credible study discovered an additional 10 grams of fiber daily reduced mortality by 17%. On average, men should consume 38 grams of fiber daily and women 25 grams. But our processed food diets fall far short of that. Most Americans consume half the amount of fiber they need. A little simple research will yield lots of foods you like to eat that are rich in fiber.
Sodium salt, the universal flavor enhancer, is used in every pre-prepared food we buy. One can of supermarket soup alone usually contains half of our daily need for sodium. (Read the labels.) Your goal should be about 1500 milligrams a day, the equal of about one teaspoon. Look at the nutritional labels at the supermarket and you’ll find that you are consuming two to six times the amount of sodium your body requires.
Too much salt leads to water being stored in your tissues. Which in turn raises your blood pressure and overworks your heart. My smart cardiac physical therapy nurse, said she had one patient (her worst case) who was so bloated that cutting back her sodium intake to normal levels led her to lose 50 pounds in one month!
Cutting back salt is a simple and powerful step to health.
Note: Simple salt reduction can be had by switching to “real salt.” Or if you are a salt addict, which many of us are, you can always try potassium salt which is sold in grocery stores. Potassium and sodium should be in balance in your body at a ratio of one to two. But be careful. Too much potassium can cause arrhythmia and other problems.

As good as new: Jeff Nightbyrd, right, with editor Thorne Dreyer at Rag Blog event in October 2014. Photo by Carlos Lowry /
The Rag Blog.
A spiritual note
After your sternum is sawed in half and your chest split open like a lobster shell, the fun stuff begins. Surgeons make incisions, and insert plastic tubes that run into a heart-lung machine. Your heart and lungs are stopped for something like an hour and a half. Get that: your heart and lungs are stopped! This means some parts of your body experience death. Nothing in our evolution has prepared us for a surgeon to stop our heart and lungs and then later use electroshock to get them functioning again. It’s very Frankenstinian, if that’s a word. You’re functionally dead and reanimated.
The eleventh morning after surgery, I woke up and was startled to feel that I had flowed back into my body. Before, I had felt like a piece of tenderized meat, beaten by a heavy kitchen mallet, prepared for frying. I realized that until that morning, the me of me had been floating just above my body. My perception of pain had been from the outside. The pain was down there.
One could argue that the Hydrocodone made my perceptions loopy.
One could argue that the Hydrocodone made my perceptions loopy. But by 10 days post-op, my thoughts and conversation seemed close to normal. Just as some people who have died remember the experience of floating out of their body, sometimes passing through a tunnel toward a white light, then looking back at themselves and feeling compelled to return, I felt the Frankenstein effect of residing just outside my body, then almost two weeks later settling back inside.
Conclusion
I have a dumbass but very good friend who is a bit bloated, doesn’t exercise, and smokes. But let it be said he is a bang-up computer programmer. Was he worried about his health? Hell no: “I’ll just have bypass surgery like you and my father.”
Pain aside, what a terrible idea for a person who works with his brain!
Avoid it.
Some of the cardiac rehab patients I exercise with are depressed and ask, “Why me?”
Outside of the philosophical question of why should we expect life to be just, one could feel: “Great, with my new blood vessels I won’t have a heart attack. Now I’m looking at another 20 years of active life. I am lucky.”
Why not you too?
[Jeff Shero Nightbyrd, who lives in Austin, was a leading figure in the ’60s New Left. He was national vice president of SDS and later was active with the Yippies. Jeff helped start Austin’s historic underground newspaper, The Rag, and was publisher and editor of RAT in New York and the Austin Sun. In recent years Jeff has run a major talent agency.]




















Just happy you are doing well,and what a great, informative session I just read. Good for you, Jeff, I am so glad you are well, and I am heeding and passing on your story and information to everyone I know. Thanks!
Hi Jeff, former Chicago office and house mate,
Tremendous article. You were always a great writer. I still remember “Deep in the Heart of Texas, the Guns of August.”
It was wonderfully useful for you to share what you learned from such a scary existential experience.
You probably already know about it, but if not, watch Forks Over Knives (on Netflix) for one approach to preserving the heart. It persuaded me to become a low-fat vegan about five months ago.
Best wishes,
Jim Russell
Great hearing from you!
Forks Over Knives has had a great impact. Even on me. Salud.
This veteran of the original Underground Press (though much more obscure) was glad to learn that you made it. Many blessings to you.
Several million people in North America have heart surgery every year. Makes my experience pretty ho-humnn,
I wrote this to send to friends who will know someone facing this crises. Cardiologists are concerned about keeping your ticker ticking. Not about your post-op quality of life. There are 2 major secrets that are rarely shared and which are largely preventable,
1. More that 50% of open heart surgery patients face clinical depression – often for months – even if they have never suffered depression before.
2. After this surgery patients suffer cognitive decline that often takes a year to recover. 20 or more points off your IQ is a concern for everyone. This is also reversible rather quickly.
So I hope people read this for tips that might improve a loved ones life, even if that loved one – as the Buddhists say – is the most difficult to love – yourself.
Correction:
The “several million” figure at the start of this note should read “about a million”.
Jeff, you’ve done a great service by writing this. Thank you.
I was wondering how you were and I guess I just found out. I hope you continue to heal. You handle it with style and a spirit of sharing for the public good. Get better comrade.
Wow, Jeffrey. Amazing story on every level. Glad you came out on the other side of this and are still here.
Hey Jeff -An excellent report. I’m happy to read that you are still among us and your reporting skills persist.
Next year is the 50th anniversary of the Tower at UT event. Any plans to commemorate? Trudy
Hey bud, glad to hear of your recovery. Last saw you at the City of Quartz and Mike Davis talk and did not know of your surgery. You looked good! glad you are back on your feet and doing well!~
This account by Jeff Nightbyrd is a wonderful way to vicariously experience open heart surgery without personally having to go through it. Such an account should inspire readers to avoid the surgery by adopting a wholesome life style. Prevention is after all the best medicine.
In Jeff’s most valuable cautions he neglected one aspect of nutrition that has come to light through peer review nutritional research. Recently found as critically involved in coronary artery occlusion is the interaction between sugar and saturated fat. These two ubiquitous components of our foods are now recognized as the primary effect in the obstruction of the arteries.
Dr. Robert Lustig gives a feature length lecture on this nutritional research, now available in a YouTube film entitled “Sugar: The Bitter Truth.” I highly recommend it. I’ve watched it three times and learn more every time I view it.
I accompanied a dear friend through his second open heart procedure. His was a valve replacement as opposed to a coronary bypass. Yet everything Jeff wrote is spot-on accurate. Thank you, Jeff. I’m so happy to know that you are all fixed up and fully recovered.
The experience I had with my friend was exceptional in that he had had the same open heart procedure when he was seventeen years of age and the surgery was still experimental–some sixty years ago. His surgeon at the time was Dr. Denton Cooley. They remained friends for life.
The open heart procedure is the last surgical specialty to be perfected. Stopping the heart and lungs was well described by Jeff. It is indeed a radical measure. You can’t operate effectively on a moving organ.
So when my friend was experiencing a return of the problems some fifty years after the first surgery he wrote to Dr. Cooley and got a referral for the best treatment available–the care of the renownd doctor’s own cardiologist. I got to sit through all the preparatory consultations and de-briefings. It was extremely enlightening. Yes, Jeff is so right about surgeons–they are extreme specialists and don’t venture beyond their expertise in the OR.
After the surgery my friend had been prescribed Amiodarone, a defibrilizing drug, and the side effects almost killed him. In researching the drug we found that 15% of those who take it do indeed die. That was an eye opener. He got a reduced dose and eventually recovered after stopping it altogether. A better dose is 200 mg and my friend had been started at 300 mg. which came close to costing him his life.
All this was over two years ago and now he is better than ever–fully recovered. His doctors told him that if he hadn’t exercised as much as he did he would not have made it through the procedure. This attests to the value of exercise.
I saw my doc a couple weeks ago. His advice was – more fiber, much less salt, and more exercise. The depression factor cannot be overemphasized; I saw it with my Dad and with friends, it is a chemical imbalance. Glad you recovered and are here to write about it. Perhaps another trip to Atlanta?
Hi Jeff,
Thank you for the article. Very sorry you had to experience this situation, but am pleased to read that you’ve turned it into a major positive for your life and those of many others. You may want to check w/ me some time to discuss herbs etc. that might be relevant to your life these daze.
Jeff, glad your back from the dead. Its a public service to relay your triple bypass story. Other folks I know have shared the awfulness of the experience. It put the fear of death in me if not the god since I’m atheist. Having read about your ordeal I’ll be sure to monitor my blood pressure, eat right, and exercise.
I hope I don’t have to have more heart surgery.
If I do I will refer to Jeff’s article.
Jeff, glad you are okay, wow, what an ordeal.
Thank you so much for the clear, informative report on your experience and all the facts the rest of us need to take into consideration.
I saw Mark Blumenthal’s reply, and highly recommend learning everything you can from his knowledge. In fact, maybe Thorne will ask Mark to write something for the Rag Blog.
Not sure that grains are the ideal fiber. Dark green vegetables and purple berries might be more effective and less troublesome on our human systems. “Grain Brain” by Dr. Perlmutter is worth reading.
I imagine your ancient Chinese doctor has some wise advice for us Rag Blog readers.
Glad you’re still alive and kicking, keep flying, Nightbyrd!
I love you, man!
Henry (formerly known as Wally)
One year after my quintuple bypass, I told my cardiologist that I didn’t want to continue taking the drugs that were keeping me zombified. The day I stopped taking Metroprolol, a beta blocker, and Lisinoprin an A.C.E. blocker, was like a rebirth. I could feel the energy that friends assumed I’d feel after the surgery. What is really frightening is that over 1/2 of people I’ve spoken to who are over sixty, are taking one or both of these energy suppressing drugs. Beta and ace blockers stop production of adrenalin. They keep blood pressure low by diminishing the life experience.
It has been over a year since I was unzombied. Trips to the gym have me feeling stronger than anytime in the last 30 years.
Coop Cooper
CAUTION: You should be very careful “telling” your cardiologist what drugs you’ll take.
I’m not a doc, but I’ve worked on preventive health for years; I assure you most docs know the basic data on medication safety, pros & cons, and would not recommend those drugs to you unless they were important to keep you alive and well.
Metoprolol, for example, is vital for those millions of us who have A-fib, rapid heartbeat which (often without us knowing we have it) can lead to stroke (and recently killed my sister at 75).
Please don’t just assume that all docs are part of the big-pharma-medical complex, making a killing from selling costly unnecessary drugs. It may kill you if you DON’T take those drugs!
So many comments attest to the fact that Jeff has indeed provided a great public service.
“Well, you’re getting older.” Don’t accept this truism if you know your body is telling you that something is not right. E.g.–Sure most of us (but not all) “slow down,” but excessive fatigue is a common symptom that is often due to drugs we’re taking–or more serious conditions. Try to get your doc to explore more.
Always question your medical providers, but respect them! If you’re really suspicious, switch!
Genetics, unfortunately, can seldom be overcome by regular exercise and a good diet. I’ve been doing most of the right things in this regard for decades but still have high blood pressure, high cholesterol, and mild plaque in both carotid and 2 coronary arteries.
But believe it, regular exercise and good diet usually make for a better quality of life and help your body tolerate treatment and ameliorate problems that come along.
Good to hear you are doing well, Jeff, and thanks again for scaring the bejeezus out of people and motivating us to do better for ourselves.
Thanks, Jeff. Now I know what to ask my cardiologist. Keep on keeping on.
Women often experience different symptoms for heart attacks. They may have chest pain or pressure, but they can also have pain in their shoulder, jaw, or arms. They frequently experience nausea; they may feel dizzy or lightheaded and short of breath; they may break out in a cold sweat; they may feel severely fatigued. There is a gender difference in response. Women are less likely to call 9-1-1; they don’t want to be a bother or disrupt family commitments; they are more likely to dismiss the symptoms as flu or heartburn because they are not the classic, chest clutching pain depicted in movies.
I’ve known two very smart women – one of them a doctor – who did not think they were having a heart related problem and waited days before getting medical attention. One of these women had nausea and shoulder pain. She saw a doctor for bursitis; a second doctor visit resulted in a diagnosis of a urinary tract infection. On the third day, a third doctor, an oncologist, called an ambulance after looking at blood pressure results. This woman died shortly after arriving at the hospital. Sisters: learn the symptoms. Don’t wait to call for help.
Terrific article with lots of detailed information. You might know that writer Larry McMurtry had heart surgery years ago. He announced at a public forum at Rice that he thought he was done with writing, suffering as you did with post operative depression. His partner pulled him out of it (I assume) by writing a book with him and in the years since he has continued to write and publish.
By the way, I know you even though you probably don’t remember me. We met in…’72…at the Republican National Convention in Miami. I was working for NPR at the time, which was still struggling to get established. I hope we can meet up sometime in Austin. Best regards!
Jeff:
I’m rereading your essay with great interest because I’m getting a triple bypass as early as tomorrow.